Abstract
Medicine Science 2015;4(2):2109-20
New Classification for Diabetic Foot Ulcers
Original Investigation
doi: 10.5455/medscience.2014.03.8215
Introduction
Diabetic foot ulcers are one of the most distressing complications of diabetes affecting around 15% of people with diabetes [4]. The annual incidence of diabetic foot ulcers is around 3% and the reported incidence in U.S and U.K studies ranges as high as 10% [5].
There are various foot ulcer classification systems that have been devised in order to categorize them more effectively and thus allow effective comparison of their outcomes in different centres [6].
The well established and most widely used ulcer classification are the Wagner’s woundclassification system and the University of Texas diabetic wound classification system [6,7].
The basic issue with Wagner’s classification is that it mixes both ulcer and gangrene and further it doesn’t mention about ischemia. UT classification is very difficult to remember and it cannot be applied in day to day practice [8].
Medicine Science 2015;4(2):2109-20
New Classification for Diabetic Foot Ulcers
Original Investigation
Need for New Classification
Various comprehensive classifications [13] have been developed over years for diabetic foot lesions. There are several well-known and accepted classification for ulcers in diabetic foot. The basic problem with Wagner’s classification is that it mixes ulcer and gangrene which are two different entities in diabetic foot. Further, there is no mention of ischaemia in the Wagner’s classification. The University of Texas classification is very complex and difficult to apply in clinical practice [8]. However the basic purpose of any classification in diabetic foot including the new proposed classification is to communicate among specialist and non- specialist equally and also to guide in therapy [14].
There is well known difference in diabetic foot between Asian and Caucasian population [15]. It hence becomes necessary to have a separate classification for diabetic foot ulcer which is distinct from the existing classification [15]. In field of diabetic foot, most specialists looks at a classification that will predict an outcome for any given treatment [16]. This should be avoided in modern practice of diabetic foot knowing that diabetic foot is multifactorial. Not only the local effect of the lesion and its extent, but even the systemic complications of diabetes and socioeconomic status of the patient have an impact on diabetic foot treatment and outcome especially in developing and underdeveloped countries. Further, the expertise of the treating doctor also plays a crucial role in final outcome of diabetic foot. In such scenario, no single classification can satisfy the researchers looking for a perfect classification that predicts outcomes an there shall never be any consensus.
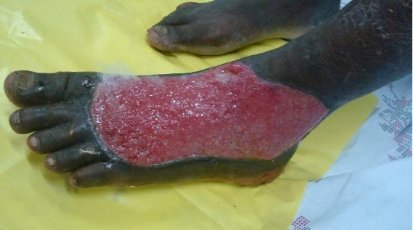
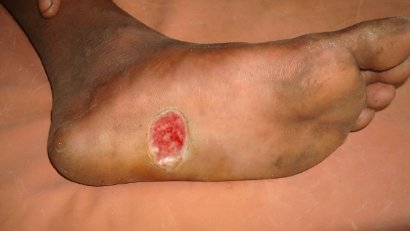
The New Classification for Diabetic Foot Ulcers
| Class 1 diabetic foot ulcers | Simple ulcers |
| Class 2 diabetic foot ulcers | Complex ulcers |
| Class 3 diabetic foot ulcers | Complicated ulcers |
Medicine Science 2015;4(2):2109-20
New Classification for Diabetic Foot Ulcers
Original Investigation
Medicine Science 2015;4(2):2109-20 New Classification for Diabetic Foot Ulcers Original Investigation
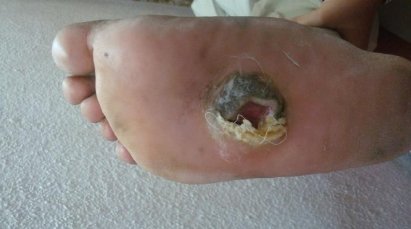
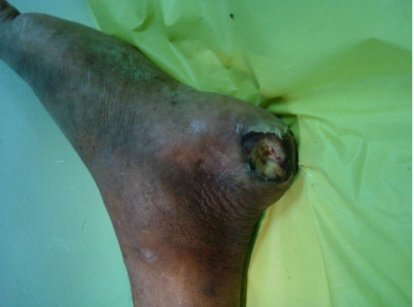
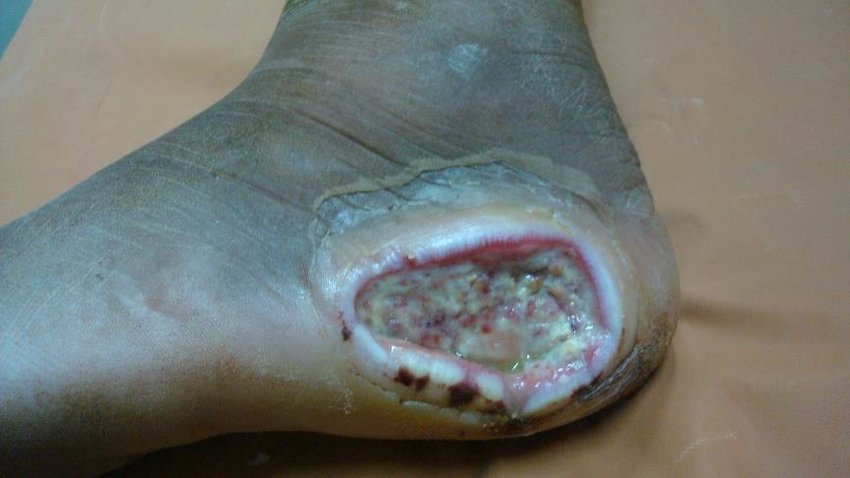
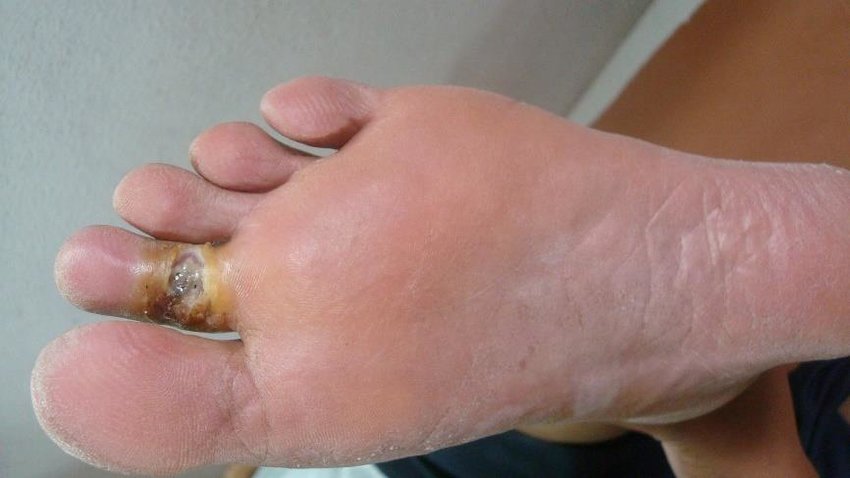
Class 3 diabetic foot ulcers are complicated diabetic foot ulcers. Such ulcers have underlying infections like abscess (Figure 5 and 6) and osteomyelitis. These ulcers require immediate surgical intervention in case the infection has to be arrested in order to prevent rapid progression.
Medicine Science 2015;4(2):2109-20 New Classification for Diabetic Foot Ulcers Original Investigation
Medicine Science 2015;4(2):2109-20 New Classification for Diabetic Foot Ulcers Original Investigation
Advantages of This New Classification
1] It is very simple
2] Easy to understand even by non-specialist and paramedical staffs like nurses
Exclusion criteria
Understanding these Ulcers
Trophic/callus ulcers without foot deformities fall in category of simple diabetic foot ulcers as a good wound care and offloading can heal these ulcers. Many a times these trophic ulcers recur due to walking on it and such cases require strict offloading.
Ischaemic ulcers that do not show wound healing with good wound care and non-interventional modalities require revascularization procedures like peripheral angioplasty or vascular bypass procedures. Ulcers with mild peripheral arterial disease may not require revascularization if with good wound care they show signs of healing. Some ischaemic ulcers are not amenable for any revascularization procedure. In such cases all possible adjunctive measures can be attempted for limb salvage.
Few ulcers may have necrotic patch (following trauma or silencer burns). They may not be infected. Simple debridement or removal of it can result in wound healing. These ulcers can be grouped under class 1. Ulcers caused due to bony prominence like Charcot foot, claw toes, hammer toes etc. are class 2 diabetic foot ulcers and they require corrections.
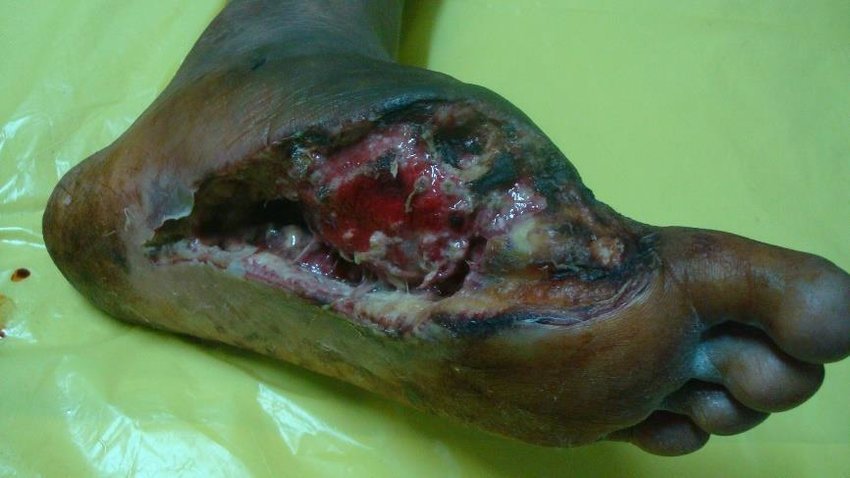
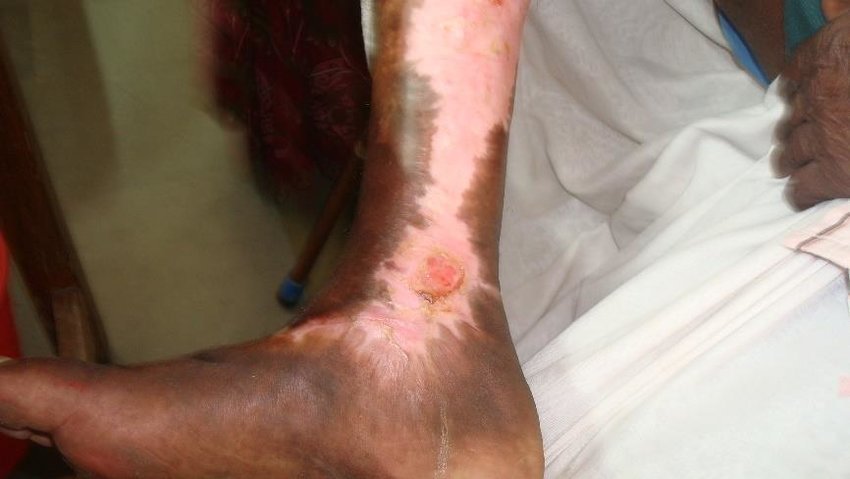
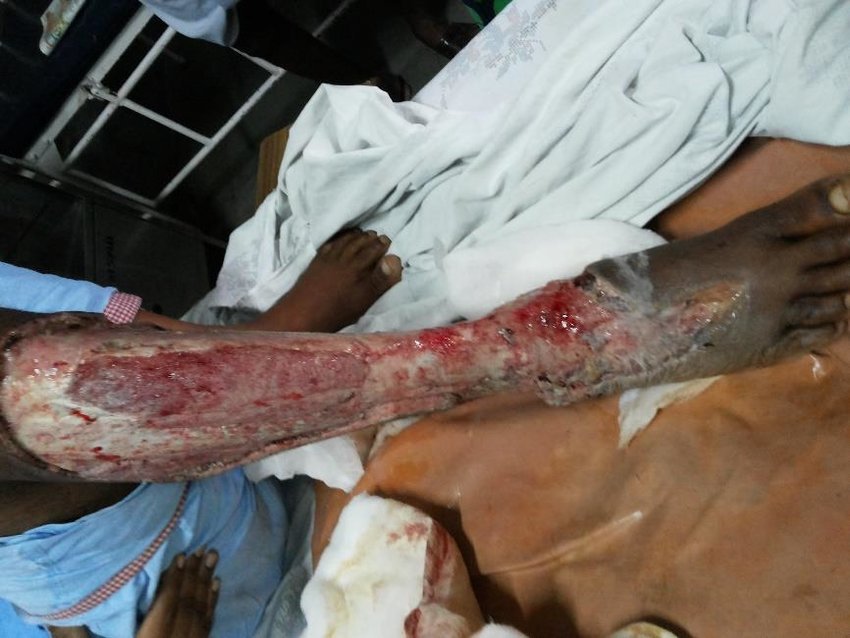
An ischaemic diabetic foot ulcer when infected secondarily becomes complicated diabetic foot ulcers (Figure 7). Such diabetic foot ulcers are at very high risk for amputation. Some ischaemic diabetic foot ulcers occur following trauma or after debridement or amputation of dry gangrene of the toe.
Venous or varicose ulcers even in diabetics should not be included in this classification.
Discussion
Diabetic foot ulcers pose a major public health problem worldwide and they are known to cause significant morbidity and mortality in diabetic patients [17]. It has been reported that 85% of the lower limb amputations in diabetic patients are preceded by foot ulceration [18,19].
A diabetic foot ulcer is considered to be a pivotal event in the life of a person with diabetes and a marker of serious disease and comorbidities [20]. Individuals who develop a diabetic foot ulcer are at greater risk of premature death, myocardial infarction and fatal stroke than those without a history of diabetic foot ulcer [20].
The diabetic foot ulcers pose a therapeutic challenge even to the surgeons especially in developing countries where health care resources are limited and the vast majority of patients present to health care centre with advanced foot ulcers [17].
Diabetic foot ulcers are prone for infections, chronicity and recurrence which eventually affect the mental health of patients [4]. Over 50% of the ulcers become infected resulting in high rates of hospitalization, severe morbidities and potential lower extremities amputation [21]. Around 14 to 24% of diabetic foot ulcers will end up in amputation [22].
In fact, in one of the series from the best limb salvage centre in India [23], around 29.4% of the patients who underwent below knee amputation had a diabetic foot ulcer (infected/non-healing) and this was the commonest cause for below knee amputation.
Although there are various classifications for diabetic foot ulcers like Wagner’s, University of Texas, S(AD)AD system, etc. [8], the author proposes another classification system for diabetic foot ulcers that is not only simple but also easy to understand. It includes most of the ulcers in diabetic foot that is commonly encountered in day to day practice. This classification could also be used as a teaching tool among different grades of specialist and non-specialist across different countries for simplifying diabetic foot practice.
Addition of this new classification by the author is another new concept and it will facilitate in development of the new “Amit Jain’s Principle and Practice of diabetic foot” that will
Medicine Science 2015;4(2):2109-20 New Classification for Diabetic Foot Ulcers Original Investigation
improvise and standardize the diabetic foot practice [11,12,24,25]. The classification is named on the author to avoid reduplication and plagiarism of this innovative work.
Conclusion
Diabetic foot complication like infection, ulceration and gangrene are common reason for inpatient admission in diabetes. Various classifications exist for diabetic foot ulcer. The new diabetic foot ulcer classification is an addition to this ulcer classification and it forms a component for the author’s new principle and practice of diabetic foot that shall improvise the diabetic foot as it is a neglected entity in underdeveloped and developing countries.
Conflict of Interests
References
9. Jain AKC, Joshi S. Diabetic foot classifications: Review of literature. Med-Science.\ 2013;2(3):715-21.
.


One Response
Hi, this is a comment.
To get started with moderating, editing, and deleting comments, please visit the Comments screen in the dashboard.
Commenter avatars come from Gravatar.