INTRODUCTION
Foot wounds are one of the most common complications seen
in patients with diabetes [ 1, 2]. Foot ulceration in diabetes is
an important precursor to amputation [3]. Peripheral
neuropathy represents the most important risk factor for the
first time foot ulceration, predisposing the foot to acute or
chronic injury [4]. Mechanical trauma is a key factor for
causing foot ulceration [5]. Foot ulcers in fact are caused by
an imbalance between excessive pressure at the plantar aspect
and cycles of repetitive stress resulting from daily ambulation
[6]. Redistribution of the plantar pressure, which is commonly
referred to as “offloading” has shown to result in faster
healing of uncomplicated neuropathic foot ulcers [5]. Thus
pressure offloading is central to achieve a good wound healing
thereby minimizing the risk of amputation [4].
CURRENTLY AVAILABLE PRESSURE OFFLOADING DEVICES/METHODS
Offloading is now recommended as a primary therapy for
prevention and management of ulcers [5]. The pressure
offloading may be achieved by a variety of means [4]. The
various available methods are bed rest, crutches, wheel chair.
Walkers, half shoes, therapeutic shoes, healing sandals, total
contact casts(TCC), removable case walkers, felted foam,
samadhan system , etc [4, 6, 7]. Each of these devices has
been used in different regions with an aim of achieving wound
healing in diabetic foot wounds. However, the evidence of
effectiveness of some of these offloading modalities is limited
[5].
SHIFTING TOTAL CONTACT CASTING FROM GOLD STANDARD TO LAST RESORT
Total contact cast offloading has been considered for years by
many to be a gold standard for ulcer offloading [ 5, 6, 8, 9].
TCC has been effective in offloading diabetic foot with
reduction in peak pressure at forefoot up to 87% [10]. TCC
has been frequently reported as effective in treating plantar
diabetic foot with healing ranging from 72% to 100% in times
ranging from 1 month to several weeks [9]. TCC has been
used in offloading diabetic foot ulcers since 1960 [8].
However, there are many problems with total contact cast. It is time consuming to apply, require expertise. It can cause skin ulcers, impacts patients lifestyle, is expensive and it cannot be used in infected wounds, causes postural instability [8, 9, 10]. Wu et al showed that only 2% used TCC in their practice [6]. Today there are various offloading methods that can be used especially for forefoot ulcers before using TCC. Hence instead of considering it as a gold standard, the author believes that is should be considered as a last resort, especially when the ulcer fails to heal with other offloading modalities.
However, there are many problems with total contact cast. It is time consuming to apply, require expertise. It can cause skin ulcers, impacts patients lifestyle, is expensive and it cannot be used in infected wounds, causes postural instability [8, 9, 10]. Wu et al showed that only 2% used TCC in their practice [6]. Today there are various offloading methods that can be used especially for forefoot ulcers before using TCC. Hence instead of considering it as a gold standard, the author believes that is should be considered as a last resort, especially when the ulcer fails to heal with other offloading modalities.
ACCOMODATIVE PADDING
Various materials have been used to temporarily offload the
wound in the foot [2]. These can be applied around the wound.
The best known accommodative padding is felted foam[2].
They are also known as deflective padding whose aim is to
deflect the pressure from the ulcer site [4]. Various other
materials have also been used to offload the wound. They
include foam mattress, roller gauge, sponges, hospital wastes
like gloves, rolled handkerchiefs, etc.
Samadhan system is one such system that utilizes cylindrical mattress foam of density 40 and it is adhered to foot using elastocrepe bandaging [7, 11]. Subsequently, other materials were also used like roller gauge, waste gloves, rolled up pads, etc to offload the ulcer. Most of these were attempted to mimics the concept of deflective padding like felted foam.
Samadhan system is one such system that utilizes cylindrical mattress foam of density 40 and it is adhered to foot using elastocrepe bandaging [7, 11]. Subsequently, other materials were also used like roller gauge, waste gloves, rolled up pads, etc to offload the ulcer. Most of these were attempted to mimics the concept of deflective padding like felted foam.
FELTED FOAM
Felted foam padding are often been used in diabetic foot
centre’s for offloading wounds especially at forefoot [4]. The technique involves adhering a felt or felted foam to the sole of
the foot, with an aperture [U shaped or circular] cut into the
material which corresponds to the location of ulcer [13]. The
aperture was cut 5 mm larger than wound with all edges
beveled [4]. Felted foam is found to be effective in offloading
ulcer though was found to be lower than TCC. It however had
advantages over TCC like allowing patient activity, could be
used in infection, allowed frequent dressing change, etc [4].
One concerned with accommodative felt dressing was edge effect [2]. Although measures were not made on diabetic with wounds, one needs to be cautious of it [2]. Another issue with felted foam is that its pressure relief properties last only up to 3 days after which it is ineffective [14].
One concerned with accommodative felt dressing was edge effect [2]. Although measures were not made on diabetic with wounds, one needs to be cautious of it [2]. Another issue with felted foam is that its pressure relief properties last only up to 3 days after which it is ineffective [14].
AMIT JAIN OFFLOADING SYSTEM/ TECHNIQUE
The author developed a new technique [one can also call it a
device or a system] that could be considered a better
alternative to felted foam for a variety of reasons. One is a
bottoming of the felted foam. It also cannot be utilized in
patients with friable skin or dermatological disorders [15].
Also, it is not available in many developing and
underdeveloped countries where it needs to be imported from
the west. Further, it is likely to be ineffective in obese patients
where it can be completely be compressed by patients body
weight
The author thus devised a new technique of offloading that addresses the above issues. It utilizes viscoelastic materials like EVA and Microcellular rubber in creating an offloading device. This offloading can be used in ulcers, postoperative wounds and also to protect the scars from breakdown at plantar area.
The author thus devised a new technique of offloading that addresses the above issues. It utilizes viscoelastic materials like EVA and Microcellular rubber in creating an offloading device. This offloading can be used in ulcers, postoperative wounds and also to protect the scars from breakdown at plantar area.
STEPS OF MAKING AMIT JAIN’S OFFLOADING SYSTEM
1] Cut a square/ rectangular piece of 3 mm microcellular
rubber sheet of appropriate size required for offloading
2] Cut an equivalent size [Figure 1] of 4mm of ethyl vinyl acetate viscoelastic elastomer [EVA]. One can also use two pieces of 2mm.
2] Cut an equivalent size [Figure 1] of 4mm of ethyl vinyl acetate viscoelastic elastomer [EVA]. One can also use two pieces of 2mm.

Figure 1 showing the Ethyl vinyl acetate(brown) and
microcellular rubber (black) cut in
2 small rectangular pieces of equal size.
2 small rectangular pieces of equal size.

Fig 2: showing necrotizing fasciitis. This is also Amit Jain’s type 1
diabetic foot complication
3] Stick both of these pieces with rubber adhesive [Figure 2
and 3].
4] Apply 2 to 3 small pieces of adhesive elasto crepe adhesive
bandage to EVA. This is to adhere to the skin of the plantar
aspect of the foot. Elasto crepe bandage is frequently used in
surgical patients and is easily available [Figure 4].

Figure 3 showing joining of both these pieces

Figure 4 showing application of 2 small pieces of adhesive
elastocrepe adhesive bandages to the EVA side of the
offloading device. This is used to adhere this device to the
skin or dressing. One can use more small pieces of bandage if
needed. It is ready to be used.
5] Then place this device at the sole of the foot [Figure 5]

Figure 5 showing the application of Amit Jain’s offloading
device. One can apply over the dressing or before the dressing
on the skin.
6] An aperture can be created to accommodate the ulcer just
like the one uses in felted foam technique. Alternatively, those
who don’t want to create an aperture can place the device
proximal to the ulcer in forefoot or distal in hindfoot ulcer.
7] Apply a large piece of elastocrepe adhesive bandage over it
to secure it firmly[ Figure 6].
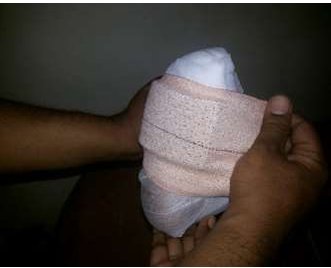
Figure 6 showing the firm securing of the Amit Jain’s
offloading device with elasto crepe adhesive bandage.
8] One can do a small dressing over the wound then used this
device or one can apply this device and then do the dressing
based on surgeon’s preference and status of the wound.
One can reuse this device by separating it from elasto crepe
adhesive bandage [dynaplast] and applying a new dynaplast.
Alternatively, it can be wrapped in roller gauge before
applying the adhesive bandage. Later it is easy to separate
from it and reuses it. The author doesn’t advocate the reuse in
exudating wounds.
References
The author devised this new offloading method based on
previous evidences. Felted foam has well known evidence in
reducing plantar pressure and healing ulcers. Deschamps et al
[16] found in his study that peak pressure reduction occurred by 50% in forefoot with felt. Felted foam gained clinical
interest to offload as it can be easily customized to the
morphology of an anatomical area. Immediate pressure
reduction with this tiny dressing has been between 30 to 60%
[16]. Various size of felted foam has been used in literature
ranging from 5 mm to 10 mm thickness [4, 13]. Curran et al
[13] found in their study that 7 mm felt padding produces
greater reduction in pressure than 5mm felt padding. They also
found that peak pressure decreased even at the edge of the
cutout. Another study [17] also supported that apertures can be
very effective for decreasing localized pressure under
metatarsal head.
Viscoelastic materials came into widespread use as insoles in
footwear because of their pressure reduction properties [18,
19]. The commonly used viscoelastic materials are
microcellular rubber, plastazotes, ethyl vinyl acetate, poron,
silicon rubber, etc [17, 18, 19, 20, 21].
Microcellular rubber (MCR) of shore hardness of around 150 shores A is known to prevent high pressure points and known to avoid plantar ulcers in anesthetic feet [20]. The cushioning property of MCR reduces force which in turn reduces pressure over the plantar surface [21]. MCR stretches in all directions and has a ability to spring back to its original shape when pressure is released while walking [20, 22]. MCR is a specially processed rubber material with 15 chemicals where air bubbles are introduced into the rubber creating millions of microcells containing air, resembling fat filled cells of sole of the foot [23]. The MCR withstands friction while walking and still maintain its thickness, elastic recoiling and it will not tear easily [23]. 3mm and 10 mm MCR are available in various South East Asian countries.
Microcellular rubber (MCR) of shore hardness of around 150 shores A is known to prevent high pressure points and known to avoid plantar ulcers in anesthetic feet [20]. The cushioning property of MCR reduces force which in turn reduces pressure over the plantar surface [21]. MCR stretches in all directions and has a ability to spring back to its original shape when pressure is released while walking [20, 22]. MCR is a specially processed rubber material with 15 chemicals where air bubbles are introduced into the rubber creating millions of microcells containing air, resembling fat filled cells of sole of the foot [23]. The MCR withstands friction while walking and still maintain its thickness, elastic recoiling and it will not tear easily [23]. 3mm and 10 mm MCR are available in various South East Asian countries.
Various different viscoelastic materials have different
properties. But from clinical point of view, these materials
have a ability to redistribute the force beneath foot, thereby
reducing pressure in the area of the foot [19]. Viscoelastic
materials like polyurethane, EVA, polyethylene, etc have good
shock absorbing properties. They are soft and light. But there
is a tendency to bottom at moderate loads unless a
considerable thickness is used, but more thickness is seldom
practical [24]. These however bottom out over months of
usage unlike felt which bottom out within 3 days.
RATIONALE FOR USING AMIT JAIN’S OFFLOADING DEVICE/ SYSTEM
With knowing the concept of deflective padding, the
advantages and disadvantages of felted foam is well known.
Since 7mm felted foam [13] is good enough to reduce greater
pressure reduction compared to 5mm, the author combined a 3
mm microcellular rubber along with 4 mm of EVA which is
commonly available all over the world. In a study by Hissink
et al, 8mm thick felted foam was used and they found that
91% of their ulcers healed in a mean time of 34 days [25].
EVA is available in 2mm, 5 mm and 10 mm thickness and is
better used as insoles in shoes of Shore 15o on an average
[ranging from 12 to 200 shore]. One can also combine 3mm
MCR and 5mm EVA to produce 8 mm thick Amit Jain’s
offloading device.
Combining 3 mm MCR and 4mm EVA produces 7 mm thickness that can be used to replicate 7mm Felted foam [Figure 7 and 8].
Combining 3 mm MCR and 4mm EVA produces 7 mm thickness that can be used to replicate 7mm Felted foam [Figure 7 and 8].
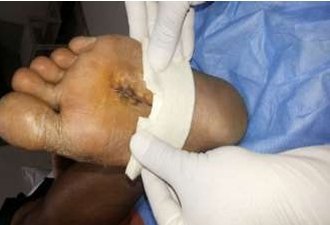
Figure 7 showing how felted foam is normally used
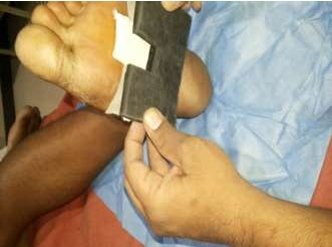
Figure 8 showing the Amit Jain’s offloading device in similar
way like felted foam. Here both MCR and EVA are black in
colour.
EVA, which is the first layer, provides a smooth, light
weighted, soft, effective cushioning and shock absorption
properties. It however can completely get compressed in 2mm
or 5mm thickness when used alone in patients with
overweight. Further there is delay in complete reformation
recovery after compression is reversed. So if patient stands for
prolong period and sufficient period or if patient is
overweight, there can be chances of EVA or other materials
like polyurethane and polyethylene in losing its purpose. This
is an undesirable property referred to as “compression set”
[19]. In such scenario, the second layer of 3 mm MCR comes
to its rescue. High pressure or prolonged pressure can produce
a greater indent in 2mm or 5mm thick EVA or other materials
which is to be avoided in presence of ulcer/ wounds. The
underneath 3 mm MCR undergoes minimal distortion,
stretches effectively in all direction and resumes to its shape
immediately [22], withstanding the friction and maintaining
its thickness without allowing the ulcer to touch the ground or
the underneath hard surface.
Thus this new Amit Jain’s offloading system or technique, which is a combination of viscoelastic material is lightweighted , can be shaped in rectangular or square shape with or without aperture in similar concept of felted foam. It is durable with shock attenuation capabilities and has good physical and mechanical properties with well defined and controllable thickness with measurable hardness. This thus forms an excellent material for offloading with deflective padding concept.
The Amit Jain’s offloading system/ device is capable of distributing inevitable forces and provides an excellent pressure relieving device for ulcer healing. This offloading technique is safe, physiological, scientifically characterized with optimiz capability.
Thus this new Amit Jain’s offloading system or technique, which is a combination of viscoelastic material is lightweighted , can be shaped in rectangular or square shape with or without aperture in similar concept of felted foam. It is durable with shock attenuation capabilities and has good physical and mechanical properties with well defined and controllable thickness with measurable hardness. This thus forms an excellent material for offloading with deflective padding concept.
The Amit Jain’s offloading system/ device is capable of distributing inevitable forces and provides an excellent pressure relieving device for ulcer healing. This offloading technique is safe, physiological, scientifically characterized with optimiz capability.
DISPLACING THE EXISTING MATERIALS
With the above known characteristic of Amit Jain’s offloading
system that is scientifically rationale, the currently used
materials like rolled up pads, roller guage, hospital wastes like
gloves, foam mattress, rubber tyres, etc used by different
people for offloading shall be henceforth displaced. Although
these materials were used with an aim of offloading diabetic
foot ulcers at an economic and rural set up where earlier good
materials were not available for offloading, the current era
requires scientifically characterized and acceptable material
with a rationale use of the concept (deflective padding) and
the viscoelastic materials are now easily available.
VARIATIONS OF AMIT JAIN’S OFFLOADING DEVICE / TECHNIQUES
The author currently used Micro cellular rubber and Ethyl
vinyl acetate as they are easily available and affordable in
many countries and they come in different color.

Figure 9 showing the combination of polyurethane with
microcellular rubber.

Figure 10 showing the easy accommodation of the Amit Jain’s offloading device along with dressing in the footwear.
Any other viscoelastic/ elastic materials like polyurethane,
polyethylene, etc used in isolation or in combination [Figure
9] in thickness of acceptable range like felted foams should be
considered to be a variation of Amit Jain’s offloading system/
technique [AMIT JAIN’S LAW]”. These would serve to be a
better alternative to felted foam in offloading diabetic foot
wounds.
ADVANTAGES OF AMIT JAIN OFFLOADING SYSTEM
1] Simple
2] Easy to prepare and applied
3] cost effective world wide
4] Can be accommodated in therapeutic foot wear [Figure 10]
5] Compliance can be considered to be partially forced as patient cannot remove it till he removes the dressing
6] It can be used in infected wounds or highly exudating wounds
7] Patient is mobile and can also do day to day activity [but should be restricted]
8] Most importantly this offloading system has defined properties and characteristics unlike any other materials
9] Based on concept of deflective padding like felted foam, this offloading system is scientifically rationale
10] It can be used in non diabetic foot wounds or for protecting sutures/ scars.
2] Easy to prepare and applied
3] cost effective world wide
4] Can be accommodated in therapeutic foot wear [Figure 10]
5] Compliance can be considered to be partially forced as patient cannot remove it till he removes the dressing
6] It can be used in infected wounds or highly exudating wounds
7] Patient is mobile and can also do day to day activity [but should be restricted]
8] Most importantly this offloading system has defined properties and characteristics unlike any other materials
9] Based on concept of deflective padding like felted foam, this offloading system is scientifically rationale
10] It can be used in non diabetic foot wounds or for protecting sutures/ scars.
CONCLUSION
Felted foam is most commonly used offloading method in
clinical practice in some of the western countries with proven
scientific evidence. It however bottoms out and loses its
property within 3 days/ much earlier. It also doesn’t have
elastic properties, shock attenuation capabilities and gives way
to higher pressure especially in overweight/obese patients.
Other materials that are used to offload like roller guage, foam
mattress, hospital waste like gloves etc have no defined
properties. They have no defined thickness, compressing
properties or measurable hardness with elastic recoiling. They
are scientifically unacceptable material in today’s era of
evidence based practice and indeed a few of this material
could serve as a foreign body in the foot.
Amit Jain’s offloading device/ system is a new offloading technique that uses scientifically acceptable material with defined properties and that utilizes the concept of deflective padding which is also a known scientifically proven method of offloading where felted foam is used. The Amit Jain’s law clearly states that “Any viscoelastic/ elastic materials like polyurethane, polyethylene, EVA, etc used in isolation or in combination in thickness of acceptable range like felted foams should be considered to be a variation of Amit Jain’s offloading system/ technique”. This offloading system can be considered to be a better and a superior alternative to felted foam.
Amit Jain’s offloading device/ system is a new offloading technique that uses scientifically acceptable material with defined properties and that utilizes the concept of deflective padding which is also a known scientifically proven method of offloading where felted foam is used. The Amit Jain’s law clearly states that “Any viscoelastic/ elastic materials like polyurethane, polyethylene, EVA, etc used in isolation or in combination in thickness of acceptable range like felted foams should be considered to be a variation of Amit Jain’s offloading system/ technique”. This offloading system can be considered to be a better and a superior alternative to felted foam.
REFERENCES
1] Deursen RV. Mechanical loading and offloading of plantar surface of the diabetic foot. CID 2004;39:587-91.
2] Foley L. Pressure point offloading in the diabetic foot.Primary intention 1999:102-108.
3] Lavery LA, Lafontaine J, Higgins KR, Lanctot DR, COnstantinides G. Shear reducing insoles to prevent foot ulceration in high risk diabetic patients. Adv Skin Wound Care 2012;25:519-24.
4] Nube VL, Molyneaux L, Bolton T, Clingan T, Palmer E, Yue DK. The use of felt deflective padding in the management of plantar hallux and forefoot ulcers in patients with diabetes. The Foot 2006;16:38-43.
5] Raspovic A, Landorf KB. A survey of offloading practices for diabetes related plantar neuropathic foot ulcers. J Foot Ank Resear 2014;7:35.
6] Wu S. Pressure mitigation for the diabetic foot ulcer. Podiatry management 2015.
7] Shankhdhar K, Shankdhar LK, Shankdhar U, Shankhdhar S. a case report: Offloading the diabetic foot wound in the developing world. J Diab Foot Comp 2011:3(2):26-29.
8] Sambrook E, Delpierre, Bowen G. Advancing the gold standard in offloading the diabetic foot. Wounds UK 2015:48 56.
9] Armstrong DG, Nguyen HC, Lavery LA, Schie CHM, Boulton AJM, Harkless LB. Offloading the diabetic foot wound. Diabetes Care 2001;24(6):1019-1022.
10] Cavanagh PR, Bus SA. Offloading the diabetic foot for ulcer prevention and healing. J Am Podiatr Med Associa 201;100(5):360-368.
11] Shankhdhar LK, Shankdhar K, Shankdhar U, Shankhdhar S. Instant offloading of a diabetic foot ulcer. CLin Res Foot Ankle 2016;4:3.
12] Kari S. The economical way to offload diabetic foot ulcers[mandakini offloading device]. Indian J Surg 2010;72(2):133-134.
13] Curran MJ, Ratcliffe C, Campbell J. A comparison of types and thickness of adhesive felt padding in the reduction of peak pressure of the foot: A case report. J Med Case Reports 2015;9:203.
14] Zimny S, Reinsch B, schatz H, Pfohl M. Effect of felted foam on plantar pressures in the treatment of neuropathic diabetic foot ulcers. Diabetes care 2001;24(12):2153-2154.
15] Giacalone V. Offloading the diabetic foot. Podiatry management 2006;253-264.
16] Deschamps K, Messier B. Pressure reducing capacity of felt. A Feasibility study using a new portable system with thin sensore. Diab Res Clin Prac 2015:e11-e14.
17] Huppin L. A new look at orthotics for diabetics. Podiatry management 2012:147-152.
18] Leber C, Evanski PM. A comparison of shoe insole materials in plantar pressure relief. Prosthetics and Orthotics International 1986;10:135-138.
19] Whittle MW, Chattanoonga. The use of Viscoelastic materials in shoes and insoles. Applied mechanics and material 2009:110-116.
20] Paul SK, Rajkumar E, Mendis T. Microcellular rubber- a boon for leprosy affected patients with anaesthetic feet in preventing secondary impairments. J Foot Ankle Res 2014;7:A92.
21] Lal V, Sarkar D, Das S, Mahato M, Srinivas G. A study to assess the usage of MCR foot wear in West Bengal, India. Lepr Rev 2015;86:273-277.
22] Enna CD, Brand PW, Reed JK, Welch D. The orthotic care of the denervated foot in Hansen’s disease. Orthotics and prosthetics 1976;30(1):33-39.
23] Thomas N, Jeyaraman K, Asha HS et al. In: A practical guide to diabetes mellitus, 6th Edition. Jaypee, India, 2012.
24] Dhanpal D, Kannan KR. PU memory foam for application as insoles in therapeutic foot wear for patients with diabetes. IJESC 2016:6(6):7784-7785.
25] Bowker JH, Pfeifer MA. In: Levin and O’Neal’s The Diabetic foot. 7th edition. Mosby, Philadelphia, 2008.
2] Foley L. Pressure point offloading in the diabetic foot.Primary intention 1999:102-108.
3] Lavery LA, Lafontaine J, Higgins KR, Lanctot DR, COnstantinides G. Shear reducing insoles to prevent foot ulceration in high risk diabetic patients. Adv Skin Wound Care 2012;25:519-24.
4] Nube VL, Molyneaux L, Bolton T, Clingan T, Palmer E, Yue DK. The use of felt deflective padding in the management of plantar hallux and forefoot ulcers in patients with diabetes. The Foot 2006;16:38-43.
5] Raspovic A, Landorf KB. A survey of offloading practices for diabetes related plantar neuropathic foot ulcers. J Foot Ank Resear 2014;7:35.
6] Wu S. Pressure mitigation for the diabetic foot ulcer. Podiatry management 2015.
7] Shankhdhar K, Shankdhar LK, Shankdhar U, Shankhdhar S. a case report: Offloading the diabetic foot wound in the developing world. J Diab Foot Comp 2011:3(2):26-29.
8] Sambrook E, Delpierre, Bowen G. Advancing the gold standard in offloading the diabetic foot. Wounds UK 2015:48 56.
9] Armstrong DG, Nguyen HC, Lavery LA, Schie CHM, Boulton AJM, Harkless LB. Offloading the diabetic foot wound. Diabetes Care 2001;24(6):1019-1022.
10] Cavanagh PR, Bus SA. Offloading the diabetic foot for ulcer prevention and healing. J Am Podiatr Med Associa 201;100(5):360-368.
11] Shankhdhar LK, Shankdhar K, Shankdhar U, Shankhdhar S. Instant offloading of a diabetic foot ulcer. CLin Res Foot Ankle 2016;4:3.
12] Kari S. The economical way to offload diabetic foot ulcers[mandakini offloading device]. Indian J Surg 2010;72(2):133-134.
13] Curran MJ, Ratcliffe C, Campbell J. A comparison of types and thickness of adhesive felt padding in the reduction of peak pressure of the foot: A case report. J Med Case Reports 2015;9:203.
14] Zimny S, Reinsch B, schatz H, Pfohl M. Effect of felted foam on plantar pressures in the treatment of neuropathic diabetic foot ulcers. Diabetes care 2001;24(12):2153-2154.
15] Giacalone V. Offloading the diabetic foot. Podiatry management 2006;253-264.
16] Deschamps K, Messier B. Pressure reducing capacity of felt. A Feasibility study using a new portable system with thin sensore. Diab Res Clin Prac 2015:e11-e14.
17] Huppin L. A new look at orthotics for diabetics. Podiatry management 2012:147-152.
18] Leber C, Evanski PM. A comparison of shoe insole materials in plantar pressure relief. Prosthetics and Orthotics International 1986;10:135-138.
19] Whittle MW, Chattanoonga. The use of Viscoelastic materials in shoes and insoles. Applied mechanics and material 2009:110-116.
20] Paul SK, Rajkumar E, Mendis T. Microcellular rubber- a boon for leprosy affected patients with anaesthetic feet in preventing secondary impairments. J Foot Ankle Res 2014;7:A92.
21] Lal V, Sarkar D, Das S, Mahato M, Srinivas G. A study to assess the usage of MCR foot wear in West Bengal, India. Lepr Rev 2015;86:273-277.
22] Enna CD, Brand PW, Reed JK, Welch D. The orthotic care of the denervated foot in Hansen’s disease. Orthotics and prosthetics 1976;30(1):33-39.
23] Thomas N, Jeyaraman K, Asha HS et al. In: A practical guide to diabetes mellitus, 6th Edition. Jaypee, India, 2012.
24] Dhanpal D, Kannan KR. PU memory foam for application as insoles in therapeutic foot wear for patients with diabetes. IJESC 2016:6(6):7784-7785.
25] Bowker JH, Pfeifer MA. In: Levin and O’Neal’s The Diabetic foot. 7th edition. Mosby, Philadelphia, 2008.

