Address of Correspondence: Dr. Ajit Kumar Varma, Professor, Department
of Endocrinology, Diabetic Lower Limb and Podiatric Surgery, Amrita
Institute of Medical Sciences & Research Center, Amrita Vishwa Vidy
Apeetham University
Elammakara, Kochi, Kerala-682041, India. Email
ajitkumarvarma@aims.amrita.edu
1 Postdoctoral Fellow in diabetic lower limb & podiatric surgery. Department
of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita
Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala,
India.
2 Professor. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
3 Podiatry Assistant. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
4 Associate Professor. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
5Professor. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
6 Professor & HOD. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
2 Professor. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
3 Podiatry Assistant. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
4 Associate Professor. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
5Professor. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
6 Professor & HOD. Department of Endocrinology, Diabetic Lower Limb and Podiatric Sugery, Amrita Institute of Medical Sciences & Research Center, Elammakara, Kochi, Kerala, India.
Introduction
Amputations are more commonly performed in
persons with diabetes than in non-diabetic
patients.1 In fact, one study reported that five out
of six amputations occurred in diabetic subjects.2
Once considered a crude mundane procedure,
amputation can be viewed as a reconstructive
procedure on par with any other limb
reconstruction.3
In the past, digital amputations were performed almost exclusively for trauma. Today, 50-70% of all non-traumatic amputations occur in diabetic patients4 and the most common cause of digital amputation is wet gangrene due to infection. Patients who have undergone digital amputation are at a greater risk of undergoing further amputation in the same limb as well as in the contralateral limb. Mortality rates at 3 and 5 years approach fifty percent in diabetic amputees, with more proximal amputations having worse survival.
The amputation rates differ widely across geographic regions within countries as well as between countries. The amputation rates range from 0.7 per 1000 in East Asian populations to 31.0 per 1000 in U.S Pima Indians.5-10 Even though the frequency of minor amputations is greater, most of the data on amputations involves major amputation. Many minor amputations such as digital amputation that usually occur in outpatient facilities are excluded when prevalence of amputation is considered. Therefore, the purpose of this study was to evaluate the incidence of digital amputations for diabetic foot infections.
In the past, digital amputations were performed almost exclusively for trauma. Today, 50-70% of all non-traumatic amputations occur in diabetic patients4 and the most common cause of digital amputation is wet gangrene due to infection. Patients who have undergone digital amputation are at a greater risk of undergoing further amputation in the same limb as well as in the contralateral limb. Mortality rates at 3 and 5 years approach fifty percent in diabetic amputees, with more proximal amputations having worse survival.
The amputation rates differ widely across geographic regions within countries as well as between countries. The amputation rates range from 0.7 per 1000 in East Asian populations to 31.0 per 1000 in U.S Pima Indians.5-10 Even though the frequency of minor amputations is greater, most of the data on amputations involves major amputation. Many minor amputations such as digital amputation that usually occur in outpatient facilities are excluded when prevalence of amputation is considered. Therefore, the purpose of this study was to evaluate the incidence of digital amputations for diabetic foot infections.
| CAUSES | NUMBER | PERCENTAGE |
|---|---|---|
| OSTEOMYELITIS | 8 | 16.67% |
| NON HEALING ULCER | 19 | 39.58% |
| GANGRENE | 20 | 41.67% |
| ABSCESS | 1 | 2.08% |
| TOTAL | 48 | 100% |
Table 1 Distribution of amputated toes by causes of amputation.
Materials and Methods
A retrospective study was carried out
from September 2008 to February 2009
in the Department of Endocrinology, Diabetic lower
limb and Podiatric surgery at Amrita Institute of
Medical Sciences, Kerala, which is a tertiary care
superspeciality hospital. All patients who had
undergone a single toe amputation were studied
during this period. Age, sex, site, side and lesion
involved were recorded. Additionally, the ankle –
brachial index [ABI] and vibration perception were
obtained. All the patients who had undergone more
than single toe amputation with or without
debridement, traumatic amputation and multiple
digital amputations were excluded from this study.
Results
A total of 114 patients had undergone
amputation (minor and major) during this
period. The minor amputations included toe
amputations, ray and partial foot amputation. The
study group consists of 48 (42.12%) of the patients
who had undergone a single toe amputation.
There was no partial amputation of toes during this
period. The average age was 61.23 years with a
range of 42 to 77 years. There were 35 males and
13 females with a ratio of 2.7:1.The distribution of
patients according to sex, side of foot, toe involved,
lesion and ankle-brachial index is summarized in
Tables 1, 2, and 3.
All the patients [100%] who underwent toe
amputation had neuropathy as detected by vibration
perception threshold whereas only 12.5% of
patients had peripheral arterial disease as measured
by ankle brachial index. The most common toe
amputation was of the great toe and the most
frequent cause of digital amputation was gangrene.
(Figure 1) The other causes were non-healing ulcer
(Figure 2), abscess and osteomyelitis with ulcer.
The 4th toe was the second most common toe that
underwent amputation. (Figure 3)
| TOES AFFECTED | NUMBER | PERCENTAGE |
|---|---|---|
| GREAT TOE | 23 | 47.92% |
| 2ND TOE | 3 | 39.58% |
| 3ND TOE | 7 | 14.58% |
| 4TH TOE | 11 | 22.92% |
| 5TH TOE | 4 | 8.44% |
| TOTAL | 48 | 100% |
Table 2 Distribution of amputation by site of amputation.
| ABI | TOES | PERCENTAGE |
|---|---|---|
| 0.9 – 1.3[NORMAL] | 42 | 87.5% |
| 0.6 – 0.89 | 26 | 12.5% |
| 0.3 – 0.59 | 0 | 0% |
| < 0.3 | 0 | 0% |
Table 3 Distribution of toe amputations according to ankle brachial index (ABI).
Discussion
The Human foot is a mechanical marvel. It
has 26 bones, 29 joints, and 42 muscles.
The bones include 7 tarsal, 5 metatarsals and 14
phalanges. The plantar pressure on a foot of a
normal man of 60 kg who is standing on one foot is
61 kilopascals. In a normal walking speed, the
plantar pressure at the 1st metatarso-phalangeal
(MTP) joint is about 299 kilopascals.11
The normal walking cycle consists of two phases; the stance phase, which takes 60% of entire gait cycle, and the swing phase, which takes 40 % of the gait cycle. The stance phase is divided into heel strike, midstance and toe off. During toe off, the great toe bears about 70% of body weight.
A mputation of the great toe leads to a disturbance in the biomechanics of the foot where the pressure is transferred to the next toe.12 A hammertoe deformity of the second toe frequently ensues and is subject to ulceration.
The prevalence of amputation in diabetic individuals is ten-fold higher compared with non diabetic subjects, 2.8% versus 0.29%.13 Foot lesions are perhaps the most common cause of hospitalization in persons with diabetes. As there is a trend towards a decline in amputations in developed countries, this is not so in the developing and underdeveloped countries.
The normal walking cycle consists of two phases; the stance phase, which takes 60% of entire gait cycle, and the swing phase, which takes 40 % of the gait cycle. The stance phase is divided into heel strike, midstance and toe off. During toe off, the great toe bears about 70% of body weight.
A mputation of the great toe leads to a disturbance in the biomechanics of the foot where the pressure is transferred to the next toe.12 A hammertoe deformity of the second toe frequently ensues and is subject to ulceration.
The prevalence of amputation in diabetic individuals is ten-fold higher compared with non diabetic subjects, 2.8% versus 0.29%.13 Foot lesions are perhaps the most common cause of hospitalization in persons with diabetes. As there is a trend towards a decline in amputations in developed countries, this is not so in the developing and underdeveloped countries.
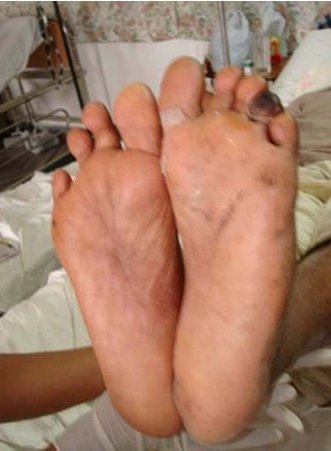
Figure 1 4th toe gangrene. There is already a 4th toe
amputation noted on the opposite foot.
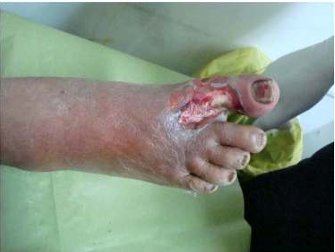
Figure 2 Non-healing ulcer of the great toe.
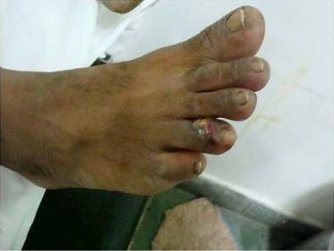
Figure 3 4th toe injury requiring subsequent
amputation.
India, with a population of greater than 1.1 billion,
reportedly has the highest number of diabetic
individuals in the world. It was estimated in the year
2000 that there were 32 million people with
diabetes mellitus in India.14 Due to a rising diabetic
population in India, the incidence of amputation is
also increasing. Furthermore, barefoot walking,
poor footwear and culture habits render the diabetic
Indian to an increased risk of amputation of the
toes.
Amputation of a single toe is associated with
complications like transfer lesions, deviation of the
toes and reulceration thereby altering the
biomechanics. (Figure 4) This renders the other
toes and the foot at a greater risk of amputation.15
When the hallux is lost due to amputation, the
weight is transferred to the 2nd toe and 2nd
metatarsal head. Approximately 65 % of hallux
amputations develop new ulcerations, with 53 %
requiring further proximal amputation.
Lesser metatarsal fractures may be seen after hallux
amputation. Amputation of the hallux results in a
reduction in the ability of the first metatarsal head
to bear weight.
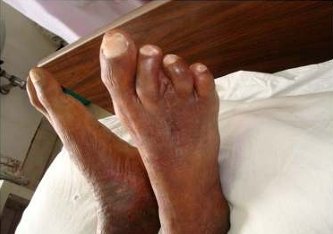
Figure 4 Deviation of toes to fill the gap after 3rd toe
amputation.
This weight is then transferred to the lesser
metatarsals. This increases the risk of lesser
metatarsal head ulceration and is associated with a
greater risk of lesser metatarsal stress fracture.16
Conclusion
Toe amputation is the most commonly
performed amputation in the diabetic foot
with the great toe being the commonest toe
(47.92%) involved followed by the 4th toe
(22.92%). Gangrene was the most frequent cause
for toe amputation. All patients who underwent toe
amputation had peripheral neuropathy as determined
by vibration perception threshold and relatively few
had vasculopathy (12.5%).
Cultural habits in India and the customary use of open footwear (sandals) contribute to the incidence of digital trauma and subsequent amputation in our patients. Although difficult in this population, behavioral and footwear changes need to be encouraged as primary preventive measures to reduce the burden of ulceration and amputation in this high-risk population.
Cultural habits in India and the customary use of open footwear (sandals) contribute to the incidence of digital trauma and subsequent amputation in our patients. Although difficult in this population, behavioral and footwear changes need to be encouraged as primary preventive measures to reduce the burden of ulceration and amputation in this high-risk population.
References
1. Bowker John H, Pfeifer Michael A.
Levin and O’Neals The diabetic foot
2008.7;1:10-11.
2. Campbell WB, Ponette D, Sugiono M. Long term results following operation for diabetic foot problems:arterial disease confers a poor prognosis. Eur J Vasc Endovasc Surg.2000 Feb;19(2):174-7.
3. Rosen RC. Digital Amputations. Clin Podiatr Med Surg 2005;22:343-363
4. Moulik PK, Mtonga R, Gill GV. Amputation and Mortality in New Onset. Diabetic Foot Ulcers Stratified by Etiology. Diabetes Care 2003;26:491 4.
5. Humphrey A, Dowse G, Thoma K, Zimmet P:Diabetes and non traumatic lower extremity amputation: incidence, risk factors and prevention: A 12 year follow-up study in Nauru. Diabetes Care 1996;19(7):710-714.
6. Lehto S, Pyorala K, Ronnemaa T, Laakso M: Risk factors predicting lower extremity amputations in patients with NIDDM. Diabetes Care 1996;19(6):607-612.
7. Morris AD, McAlphine R, Steinke D, et al: Diabetes and lower-limb amputations in the community. Diabetes Care 1998;21:738-743.
8. Nelson R, Gohdes D, Everhart J, et al: Lower extremity amputations in NIDDM: 12 yr follow up study in the Pima Indians. Diabetes Care 1988; 11:8-16.
9. Siitonen OL, Niskanen LK, Laakso M,et al: Lower extremity amputations in diabetic and non diabetic patients. Diabetes Care 1993;16:16-20.
10. Trautner C, Haastert B, Giani G, Berger M: Incidence of lower limb amputations in the Netherlands and in the state of California. J Int Med 1996; 240:227-231.
11. Rosenbaum D, Hautmann S, Gold M, Cleas l:Effects of walking speed on plantar pressure patterns and hindfoot angular motion. Gait Posture 1994;2(3):191-197.
12. Sullivan JP. Complications of pedal amputations. Clin Podiatr Med Surg 2005;22:469 484.
13. Reiber GE , Boyko EJ, Smith DG: Lower extremity foot ulcers and amputation in diabetes. In National Diabetes Data Group(ed):Diabetes in America,2nd ed(NIH publ.no.95-1468). Washington DC, U>S. government Printing Office, 1995,pp 409-428.
14. Wild S, Roglic G, Green A, et al: Global prevalence of diabetes: Estimates for 2000 and projection for 2030. Diabetes Care 2004;27:1047 1053.
15. Mann R,Poppen N, O’ Konski M. Amputation of the great toe: a clinical and biomechanical study. Clin Orthop 1998;226:197.
16. Lanucci A, Lai King P, Channell R, et al. Spontaneous fractures of the lesser metatarsals secondary to an amputated hallux and peripheral neuropathy. J Foot Surg 1987;26:66.
2. Campbell WB, Ponette D, Sugiono M. Long term results following operation for diabetic foot problems:arterial disease confers a poor prognosis. Eur J Vasc Endovasc Surg.2000 Feb;19(2):174-7.
3. Rosen RC. Digital Amputations. Clin Podiatr Med Surg 2005;22:343-363
4. Moulik PK, Mtonga R, Gill GV. Amputation and Mortality in New Onset. Diabetic Foot Ulcers Stratified by Etiology. Diabetes Care 2003;26:491 4.
5. Humphrey A, Dowse G, Thoma K, Zimmet P:Diabetes and non traumatic lower extremity amputation: incidence, risk factors and prevention: A 12 year follow-up study in Nauru. Diabetes Care 1996;19(7):710-714.
6. Lehto S, Pyorala K, Ronnemaa T, Laakso M: Risk factors predicting lower extremity amputations in patients with NIDDM. Diabetes Care 1996;19(6):607-612.
7. Morris AD, McAlphine R, Steinke D, et al: Diabetes and lower-limb amputations in the community. Diabetes Care 1998;21:738-743.
8. Nelson R, Gohdes D, Everhart J, et al: Lower extremity amputations in NIDDM: 12 yr follow up study in the Pima Indians. Diabetes Care 1988; 11:8-16.
9. Siitonen OL, Niskanen LK, Laakso M,et al: Lower extremity amputations in diabetic and non diabetic patients. Diabetes Care 1993;16:16-20.
10. Trautner C, Haastert B, Giani G, Berger M: Incidence of lower limb amputations in the Netherlands and in the state of California. J Int Med 1996; 240:227-231.
11. Rosenbaum D, Hautmann S, Gold M, Cleas l:Effects of walking speed on plantar pressure patterns and hindfoot angular motion. Gait Posture 1994;2(3):191-197.
12. Sullivan JP. Complications of pedal amputations. Clin Podiatr Med Surg 2005;22:469 484.
13. Reiber GE , Boyko EJ, Smith DG: Lower extremity foot ulcers and amputation in diabetes. In National Diabetes Data Group(ed):Diabetes in America,2nd ed(NIH publ.no.95-1468). Washington DC, U>S. government Printing Office, 1995,pp 409-428.
14. Wild S, Roglic G, Green A, et al: Global prevalence of diabetes: Estimates for 2000 and projection for 2030. Diabetes Care 2004;27:1047 1053.
15. Mann R,Poppen N, O’ Konski M. Amputation of the great toe: a clinical and biomechanical study. Clin Orthop 1998;226:197.
16. Lanucci A, Lai King P, Channell R, et al. Spontaneous fractures of the lesser metatarsals secondary to an amputated hallux and peripheral neuropathy. J Foot Surg 1987;26:66.

