Foot ulceration is one of the most common
and serious complication of diabetes and
it precedes lower-extremity amputations
in up to 80% of cases (Baker and Osman, 2017).
Plantar ulceration is a common complication
in a neuropathic diabetic foot (Armstrong et al,
2004; Deursen, 2004). This plantar ulceration
often initiates a process of further ulceration and,
ultimately, amputation (Deursen, 2004). Around
56% of diabetic foot ulcers get infected and 20%
of the patients with infected wounds end up
with some form of lower-extremity amputation
(Wu, 2015).
Knowing the fact that neuropathic ulceration
occurs because of a combination of focal pressure
and repetitive stress at a given site (Armstrong
et al, 2004), redistribution of plantar pressure
away from sites of elevated pressure (offloading)
results in faster healing of foot ulcers (Raspovic
and Landorf, 2014). In fact, uncomplicated
plantar ulcers should heal in 6 to 8 weeks with
adequate offloading (Cavanagh and Bus, 2010).
However, the author observed in clinical practice
that it can take longer to heal as it depends
upon the size of the ulcer, location of the ulcer,
recurrences, previous surgeries, type of offloading
modality used, compliance of patient, status
of the opposite limb and systemic condition of
the patient.
Various offloading methods are available in
different countries. This article describes a case of
forefoot ulcer that was healed using Amit Jain’s
offloading system (Jain 2017a; 2017b; Jain et al,
2017); a new deflective offloading system.
Case report
A 64-year-old woman with a history of diabetes
mellitus of 20 years’ duration presented to the
author’s department with a non-healing ulcer in the
right forefoot region that she had had for 3 months.
The patient was already experiencing peripheral
neuropathy and had undergone amputation of the
right big toe 3 years previously. She was treated
at multiple hospitals, but she found the ulcer was
increasing in size.
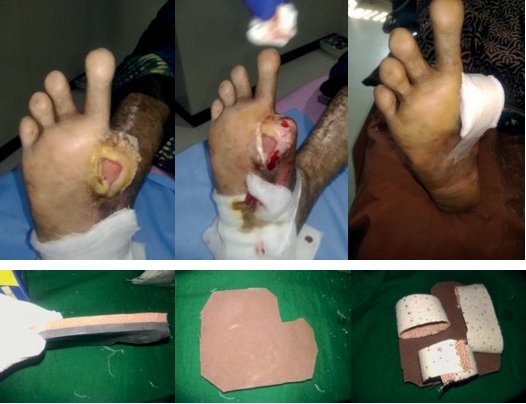
On examination, the patient was found to have
a non-healing ulcer measuring around 2.5 x 2.2 cm2
at first metatarsophalangeal joint (MTPJ) region
[Figure 1]. It belonged to Amit Jain’s S2A1C1 ulcer
type (Jain 2017c). It had pale granulation tissue
at its base with punched-out edges. There was
no probing to bone and X-ray of the foot did not
show osteomyelitis.
The wound was cleaned with povidone iodine
and saline, and surrounding callosity was debrided
[Figure 2]. A dressing was applied [Figure 3] and Amit
Jain’s offloading device was prepared and applied
as follows:
- A square/rectangular piece of 8 to 10 cm2
microcellular rubber (MCR) of 10o to 15o shore A
hardness with 3 mm thickness is prepared
- An equal size piece of ethyl vinyl acetate (EVA) of
5 mm thickness with 10o to 15o shore hardness
is prepared
- A synthetic rubber adhesive is applied and both
are stuck together. This is an 8 mm thick Amit Jain
offloader [Figure 4].
- In this case, an L-shaped aperture is made over
of the corners of the offloader, removing a small piece as shown [Figure 5] to accommodate the
area of ulcer
Figure 1 (left). Shows the non
healing trophic ulcer at first MTP
region of right foot.
Figure 2 (middle). Shows the
wound cleaned and surrounding
callosity debrided.
Figure 3 (right). Shows the wound
being dressed.
Figure 4 (left). The 8mm Amit Jain’s
standard offloading.
Figure 5 (middle). An aperture
made in offloading to
accommodate the ulcer area.
Figure 6 (right). Application of
strips of elastocrepe bandage.
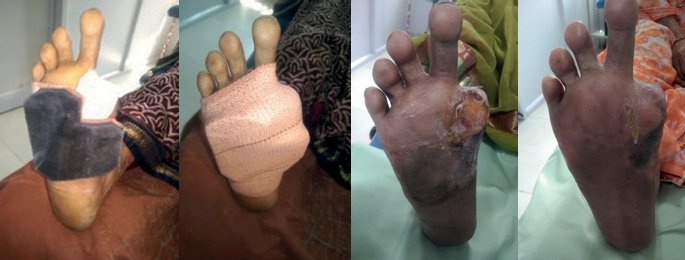
- The offloader is loosely secured by applying two
to three strips of elastocrepe adhesive bandage
on the EVA side as shown [Figure 6] and this is
anchored to the plantar skin [Figure 7]
- The Amit Jain offloader is then densely secured
by applying large elastocrepe adhesive as
shown [Figure 8]
- This offloader and dressing were changed every
3 to 4 days. The patient was allowed to use her
protective footwear with a polymer insole
- The ulcer showed significant improvement
[Figure 9] and healed at end of 7 weeks and 2
days of application [Figure 10]. We continued
using the offloading for 2 more weeks for
scar protection.
Discussion
Offloading of diabetic foot neuropathic ulcer is
recommended as one of the main modalities
for prevention and management of ulcer
(Raspovic and Landorf, 2014). In spite of its known
importance, it is often ignored and overlooked due
to lack of training, poor understanding or limited
resources (Shankhdhar et al, 2016; Baker and
Osman, 2017).
Today, offloading is one of the main
recommended treatment modality in diabetic
foot ulcers. The author believes that offloading of
foot ulcers should be considered both as an art
and science, instead of just an art (Cavanagh and
Bus, 2010).
Various offloading devices are available and
include total contact casts (TCCs), removable casts,
felt padding, Amit Jain’s offloading system, half
shoes, samadhan system, CROW and cast shoes
(Raspovic and Landorf, 2014; Jain, 2017a; 2017b).
The TCC, which was suggested earlier to be the
first line offloading and the considered to be a gold
standard in the West, is infrequently used in many
developing countries due to multiple reasons (Jain,
2017a), including non-acceptance by patients, due
to lack of knowledge and resistance to use by the
treating clinicians. TCC is strictly contraindicated in
infection, ischaemia, loss of sight and poor balance
(Baker and Osman, 2017). Furthermore, it requires
expertise, time, cost and can cause complications,
such as skin ulcers (Sambrook et al, 2015; Jain,
2017a). Even in Western countries, it was shown
that only 2% of practitioners use TCC (Wu, 2015).
TCC should be considered to be a last resort of
offloading when other modalities fail to heal the
ulcer (Jain, 2017a).
Felted foam is a commonly used offloading
method in clinical practice. Various studies have
found that 7 mm to 8 mm felted foam are effective
(Bowker and Pfeifer, 2008; Curran et al, 2015). Its
main disadvantage is bottoming and losing its
pressure-relief properties (Jain, 2017a). Furthermore,
it is not available in developing countries.
Amit Jain’s offloading system is a better
Discussion
A diabetic foot is known to produce a huge burden on the health care system worldwide. In developing countries like India, patients with foot complications spend around 32.3% of their income on the treatment.
Various studies have been done on diabetic foot using Wagner’s classification over last 3 decades. Wagner’s classification has been the most widely utilised system for lesions in a diabetic foot. The basic problem with Wagner’s classification is that it does not include all diabetic foot problems, does not describe vascular disease and there is wide distinction in the grades.
The new Amit Jain’s classification was proposed to include all the complications of a diabetic foot. It is the simplest of all the diabetic foot classifications, practical, easy to understand and can be used as a teaching tool.
This study aims to evaluate the usefulness of this classification for research studies for the first time.
Most of the studies worldwide show male predominance. In our study, males accounted for 84.44% and were affected more than females at a ratio of 5.4:1.
According to this study, type 1 diabetic foot complications are the most common complication (86.66%) and type 2 is the least common (2.22%). In fact, studies have shown that in India, most foot problems are infective and neuropathic in nature rather than vascular. In one such study, infection was as high as 90%, thereby resulting in amputations.
The rate of major amputation varies from 9–24% in literature. In our study, 8.89% of our patient underwent major amputation and all these patients belong to type 1 complications. There was no mortality in our study during this period. This may be due to the fact that less than 10% of our total operated cases were on a diabetic foot.
In this study, we found that we were able to appropriately distribute and study all the diabetic foot lesions according to this classification.
Figure 7. The application of Amit
Jain’s offloading in a similar fashion
as felted foam.
Figure 8. Firm securing of Amit
Jain’s offloading with elastocrepe
adhesive bandage.
Figure 9. The ulcer reduced in size
drastically at the end of 4 1/2 weeks.
Figure 10. The ulcer completely
healed.
alternative to felt in developing and also in
developed countries. In the standard Amit Jain’s
offloading system, a combination of 3 mm
microcellular rubber and a 4 mm to 5 mm of EVA is
used to make a 7 mm to 8 mm thick offloader that
can be used similar to felt. Microcellular rubber
(MCR) of shore hardness 10–15o shore A is known
to prevent pressure points (Jain, 2017a). It has good
cushioning properties, stretches in all direction and,
most importantly, has the ability to spring back to
its shape immediately when pressure is released in
walking (Paul et al, 2014; Jain, 2017a). It is available
in the author’s region in 3 mm and 10 mm thickness.
EVA is smooth, lightweight and soft with effective
cushioning properties.
The combination was used by the author after
conducting multiple pilot studies and observations.
Obtaining 7 mm/8 mm microcellular rubber was
difficult as the authors wanted to replicate felted
foam. It was discovered that 10 mm MCR was too
thick and there was pain and erythema after three
to four applications. The issue with isolated EVA of
7 mm or 8 mm was that in overweight and obese
patient it would get completely compressed,
leading to pressure on the ulcer. EVA has an
undesirable property referred to as “compression
set” (Jain, 2017a).
In such a situation, the author combined a 3 mm
MCR and 4 mm/5 mm EVA to produce an effective
combination wherein the MCR would come to the
rescue of compressed EVA and avoid contact of the
wound to the ground, as well as resume its shape
immediately (Jain, 2017a). Other combinations can
also be used, but it is governed by Amit Jain’s law
of offloading (Jain, 2017a; Jain, et al, 2017). This law
states: “Any viscoelastic/elastic materials used in isolation or combination in thickness of acceptable
ranges like felted foam should be considered to be
a variation of Amit Jain’s offloading system”. This law
was proposed to avoid plagiarism of this technique
Conclusion
The practice of offloading is changing especially
in developing and under-developed countries.
Various new deflective offloading devices are now
available. Amit Jain’s offloading is one such new,
simple deflective offloading, which is a better and
superior alternative to foam. This offloading system
has a scientific rationale of usage based on the
deflective offloading concept, in view of the defined
characteristics and properties of the materials used,
which are scientifically accepted worldwide
References
Armstrong DG, Lavery LA, Nixon BP, Boulton JM (2004) It’s
not what you put on, but what you take off: Technique for
debriding and offloading the diabetic foot wound. Clin
Infect Dis 39(Suppl 2): S92–9
Baker N, Osman IS (2017) The principles and practicalities of
offloading diabetic foot ulcers. Diabetic foot Canada 5(1):
28–34
Bowker JH, Pfeifer MA (2008) In: Levin and O’Neal’s The Diabetic
Foot. (7th edn.) Mosby, Philadelphia
Cavanagh PR, Bus SA (2010) Offloading the diabetic foot
for ulcer prevention and healing. J Am Podiatr Med Assoc
100(5): 360–8
Cavanagh PR, Bus SA (2010) Offloading the diabetic foot
for ulcer prevention and healing. J Vas Surg 52(3 Suppl):
37S–43S
Curran MJ, Ratcliffe C, Campbell J (2015) A comparison
of types and thickness of adhesive felt padding in the
reduction of peak pressure of the foot: A case report. J Med
Case Reports 9: 203
Deursen RV (2004) Mechanical loading and offloading of the
plantar surface of the diabetic foot. CID 39: S87–91
Expert commentary: Healing a
diabetic forefoot non-healing
neuropathic ulcer using the new Amit
Jain’s offloading system
Dabetic foot ulcers, especially non
healing ones, and their complications
not only put a massive strain on
healthcare systems the world over, but have
a major impact on the quality of life for the
patient. I have always said that healing any
diabetes foot ulcer is like ‘pulling all the pieces
of a jigsaw together’ and if all the ‘pieces’ are
not in place, it will result in non healing or, at
best, delayed healing.
In my 29 years’ experience of treating
diabetes foot ulceration, I know that the
‘piece of the jigsaw’ that is usually neglected
is pressure relief, especially in neuropathic
patients. I feel the reason for this can
be threefold:
- Patient compliance due to insensate feet
- Lack of understanding
- The varied ability to supply suitable
pressure relief
Amit quite correctly points out in his article
that Total Contact Casting ‘in the West’ is
considered to be gold standard, but even in
developed countries only 2% of practitioners
actually regularly use this treatment modality.
The reasons for this are generally related to
patient acceptance, suitable clinician training
and lack of access to a 7-day per week service.
Often, even in what we like to think of as
‘gold standard’ multidisciplinary foot clinics
in the UK, we have to make compromises,
for whatever reason, to suit either patient or
service circumstances.
As Amit points out, felt padding, although
not ideal, is still sometimes used in Western
countries as a method of offloading, but this
is not an option for Amit’s patients due to the
lack of availability of felt in India.
Sometimes as clinicians, we have to
‘adapt our treatment plan’ according to our
circumstances and, in my opinion, Amit has
done this very well.
Amit Jain’s offloading system to my mind
demonstrates very clever use of what is
available locally to achieve an end goal of
pressure relief, or at least significant pressure
reduction, to aid ulcer healing.
Amit has also very cleverly realised that
using different densities of materials in
combination not only provides enhanced
pressure-relieving properties, but also
prevents ‘bottoming out’, which happens quite
quickly with the use of a material such as felt.
In the UK, in my experience and in my
travels to other developed countries, many
removable or non-removable pressure
relieving/reducing strategies are adopted
and fitted to patients. These strategies are not
available to Amit in his clinic in India and I feel
although his offloading system does have its
limitations and drawbacks, he has introduced
a strategy with what is available to offload
his patients to the best of his ability with the
available resources.
When we look at such strategies, we should
be very grateful and understand, even though
we do moan sometimes, that actually the
service we provide, although not perfect, is
infinitely better that services that are being
provided in some other countries around
the world.