Received: 22 May 2017
Accepted: 23 June 2017
Correspondence
- Dr Amit Kumar,
- E-mail: dramitkumarcj@yahoo.in
ABSTRACT
Background: It is a well-known fact that around 15% of patients with diabetes are likely to be affected by foot ulcersduring their lifetime. The aim of this study was to evaluate and analyze Amit Jain’s offloading system used in diabeticfoot wounds.
Methods: A cross-sectional, retrospective study was done at 3 centres namely Brindhavvan Areion Hospital, SynergyCentre for Diabetes and South City hospital in Bangalore, India. The study period was for 1 year from April 2016 toMarch 2017.
Results: 23 cases were included in the study. 16 patients (69.57%) had right foot involved whereas 7 patients(30.43%) had left foot involved. Majority of the patients had foot problems located at forefoot (86.96%). The mostcommon condition where Amit Jain’s offloading was used was in trophic ulcer (61%). In 22 patients (95.65%), themicrocellular rubber and ethyl vinyl acetate combination was used whereas in one patient (4.35%), 7 mm of singlelayered EVA was used. 9 patients (39.13%) had their wounds healed within 8 weeks whereas 11 patients (47.83%)had their wounds healed within 8-16 weeks.
Conclusions: Amit Jain’s offloading device is a new offloading device that can be effectively used as an alternativeto felted foam. It is based on deflective technique just like felted foam. In this series, 86.98% of the wounds hadhealed by 16 weeks with this new offloading device. The Amit Jain’s offloading device, which has a scientificrationale based on the deflective offloading as well as usage of visco-elastic material that is accepted worldwide,produces effective wound healing without any complication and without inhibiting patient’s mobility. Amit Jain’soffloading is a level one recommendation for diabetic foot wounds.
Keywords: Amit Jain, Diabetic foot, Felt, Law, Offloading, Ulcer
INTRODUCTION
Debridement of the wound, appropriate dressings and offloading are essential for healing of ulcers.4,8
Numerous offloading methods are available and include bed rest, therapeutic shoes, felted foam, total contact casts, removable cast walkers, etc.6-11 Felted foam padding is one such offloading method used commonly in clinical practice.12 Amit Jain’s offloading technique is an alternative to felted foam used to offload diabetic foot wounds.9
The current study aims at sharing study experience with Amit Jain’s offloading system in diabetic foot wounds.
METHODS
Inclusion criteria
• All the patients with diabetic foot neuropathic ulcers
• Patients with Postoperative wounds (less than 5 cm) incision scars in diabetic foot.
Exclusion criteria
• Non-diabetic foot wounds
• Patients who lost for follow up
• Ischemic wounds
• Patients with multiple ulcers on the foot wereexcluded
• Patients whose ulcer got infected during the treatment course and ended up in amputation.
RESULTS
A total of 27 patients had received the Amit Jain’s offloading device but only 23 cases were included in the present study. 15 patients (65.22%) were males and 8 (34.78%) were females (Table 1).
The average age of males was 51.2 years and for femaleswas 49.6 years. 16 patients (69.57%) had right foot involved whereas 7 patients (30.43%) had left footinvolved (Table 2).
20 patients had foot problems located at forefoot (86.96%), 2 of whom had trans metatarsal amputation,one at midfoot (4.35%) and two patients (8.7%) at heel
(Table 3).
19 patients (82.61%) had non-healing ulcer (Trophic ulcer), one patient (4.35%) had scar dehiscence and 3 patients (13.04%) had post-operative wounds on whichAmit Jain’s offloading were used (Table 4).
The postoperative wounds (less than 5 cm) were the wounds status post debridement for diabetic foot abscess (the wounds that didn’t reach bone). Dressing was changed once in 3 to 4 days based on soakage and wounds were periodically inspected. A new offloading was used every time the dressing was changed and non
where reused in this series.
In 13 patients (56.52%), 7 mm thick Amit Jain’s offloading device (Table 5) was used (combination of 3mm microcellular rubber and 4 mm of ethyl vinyl acetate) and in 10 patients (43.48%) 8 mm thick offloader was used (3 mm MCR + 5 mm EVA).
whereas in one patient [4.35%], 7 mm of single layered EVA was used. This was purely based on availability of the viscoelastic materials during the study period. The single 7mm EVA [made by combining 5mm and 2 mm EVA] was used when the 3-mm microcellular rubber was out of our stock at our centre
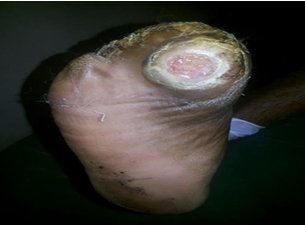
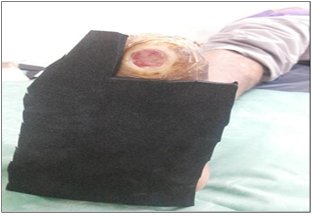
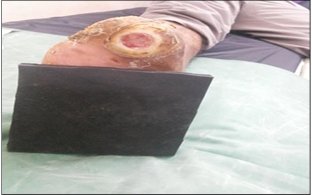
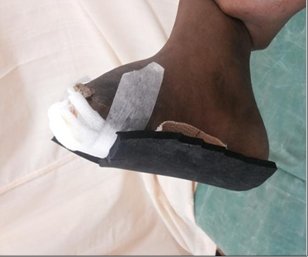
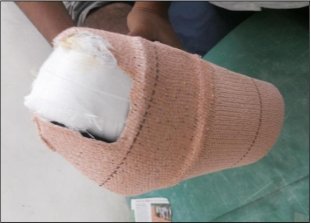
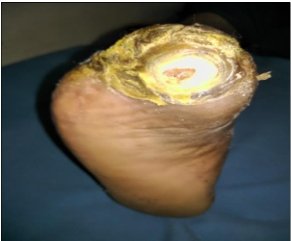
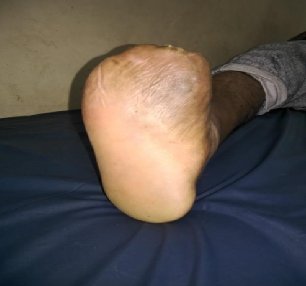

9 patients (39.13%) had their wounds healed within 8 weeks. 11 patients (47.83%) had their wounds healed within 8-16 weeks and 3 patients (13.04%) wound remained unhealed after 16 weeks (Table 6). They were subsequently put on different offloading methods like TCC and Bohler iron cast. None of these patients had
DISCUSSION
CONCLUSION
Funding: No funding sources Conflict of interest: None declared Ethical approval: Not required
REFERENCES
1. Ahmed AA. Diabetic foot: Offloading Devices. MEJFM. 2009;7(6):18-21.
2. Foley L. Pressure point offloading in the diabetic foot. Primary Intention. 1999;102-108.
3. Deursen RV. Mechanical offloading and offloading of the plantar surface of the diabetic foot. CID 2004;39:589-91.
4. Armstrong DG, Lavery LA, Nixon BP, Boulton AJ. It’s not what you put on, but what you take off: techniques for debriding and offloading the diabetic foot wound. CID. 2004;29:592-99.
5. Raspovic A, Landorf KB. A survey of offloading practices for diabetes related plantar neuropathic foot ulcers. J Foot Ank Resear. 2014;7:35.
6. Shankhdhar K, Shankhdhar LK, Shankhdhar U, Shankhdhar S. A case report: offloading the diabetic foot wound in the developing world. J Diab Foot Comp. 2011;3(2):26-29.
7. Cavanagh PR, Bus SA. Offloading the diabetic foot for ulcer prevention and healing. J Am Podiatr Med Assoc. 2010;100(5):360-8.
8. Agrawal VP, Sreeramulu PN. Most easy on the pocket offloading device costing <1 $ for rural diabetic foot ulcers. Surgery Curr Res. 2012;2:4.
9. Jain AKC. Amit Jain’s offloading system for diabetic foot wounds: a better and superior alternative felted foam. IJMSCI. 2017;4(1):2604-9.
10. Wu SC, Jensen JL, Weber AK, Robinson DE, Armstrong DG. Use of pressure offloading devices in diabetic foot ulcers. Diabetes Care. 2008;31(11):2118-9.
11. Mulder G, Alfieri D. The diabetic foot: consideration for pressure reduction and offloading. Intention. 2007;15(2):58-65.
12. Curran MJ, Ratcliffe Connor, Campbell J. A comparison of types and thickness of adhesive felt padding in the reduction of peak plantar pressure of the foot: case report. J Med Case Reports. 2015;9:203.
13. Sambrook E, Delpierre T, Bowen G. Advancing the gold standard in offloading the diabetic foot. Wounds UK. 2015:48-26.
14. Wu S. Pressure mitigation for the Diabetic foot ulcer. Podiatry Management. 2015:79-85.
15. Cavanagh PR, Bus SA. Offloading the diabetic foot for ulcer prevention and healing. J Vas Surg. 2010;52(3):375-435.
16. Nubé VL, Molyneaux L, Bolton T, Clingan T, Palmer E, Yue DK. The use of felt deflective padding in the management of plantar hallux and forefoot ulcers in patients with diabetes. The Foot. 2006;16(1):38-43.
17. Zimny S, Reincsh B, Schatz H, Pfohl M. Effect of felted foam on plantar pressures in the treatment of neuropathic diabetic foot ulcers. Diabetes Care. 2001;24(12):2153-4. Jain AKC. Amit Jain’s classifications for offloading the diabetic Foot wounds. IJMSCI 2017;4(5):29225.

