Keywords: Amit Jain’s classification, Diabetic foot, Osteomyelitis
1 MBBS, DNB, FPS – Assistant Professor, 2 MBBS, DNB – Associate Professor
Department of Surgery, St Johns Medical College, Bangalore
Corresponding author mail: dramitkumarcj@yahoo.in
INTRODUCTION
Around 15% of
diabetic patients will develop an ulcer in
their lifetime1. The ulcers are prone for
infection that can deteriorate rapidly and
involve deeper structures like bone leading
to osteomyelitis2. The term osteomyelitis
was first coined by Nelaton in 18443.
Osteomyelitis accounts for around 10
20% of diabetic foot ulcers4, 5, 6 and it can be
as high as 60%5. In spite of the fact that it
has a high frequency, treatment of
osteomyelitis of the foot continues to be
controversial and there are no optimal
treatment guidelines yet6. Further, there was
no specific classification for diabetic foot
SEAJCRR JULY-AUG 3 (4) eISSN: 2319 – 1090 Page 795
osteomyelitis for many decades. Many
studies done on diabetic foot did not even
mention about the type of osteomyelitis that
occurred in their study7, 8, 9.
Amit Jain’s classification for diabetic foot
osteomyelitis10 is the first new specific
classification for osteomyelitis occurring in
diabetic foot [Table 1]. This study aims at
analyzing the diabetic foot osteomyelitis
using
Table here
CORRESPONDING AUTHOR: Dr Amit Kumar C Jain
Table 1 showing the new Amit Jain’s classification of diabetic foot osteomyelitis.
ABSTRACT: Offloading of the wounds in the foot is one of the most important and integral part of wound management to achieve optimal successful results. Various offloading modalities have been used for decades with each having their own merits and demerits. However, astonishingly, as far as the author knows, as an expert diabetic foot surgeon, there is no classification till date that divides offloading devices in appropriate distinct group. The Author proposes new different classifications for offloading devices/system in diabetic foot for the first time in the literature. It is a novel attempt to improvise and standardize diabetic foot practices around the world and is another component of Amit Jain’s principle and practice of diabetic foot. This offloading classification can also be used for non-diabetic foot wounds.
MATERIALS AND METHOD:
A retrospective analysis was carried in the Department of Surgery of St Johns medical college, Bangalore, India, which is a tertiary care institute of repute. All the osteomyelitis cases treated by the authors were studied. The study period was from March 2011 to February 2014. The following where the inclusion and exclusion criteria. INCLUSION CRITERIA
1] Diabetes mellitus.
2] All the patients seen by the authors both as in patients as well as outpatient were included in the study.
3] Patients operated elsewhere and who came to us for further management were also included in this study
EXCLUSION CRITERIA
1] Non diabetics.
2] Patient treated in other units or department were excluded.
3] Patients with incomplete data were excluded from the study.
RESULTS
A total of 21 patients with diabetic
foot osteomyelitis were included in this
study. There were 14 males [66.67%] and 7
females [33.33%]. The average age for
males was 49.2 years with age ranging from
39 years – 66 years and average age for
females was 51.5 years with age ranging
from 41 years – 64 years. 20 patients
[95.23%] had unilateral osteomyelitis and one patient [4.76%] had bilateral
osteomyelitis.
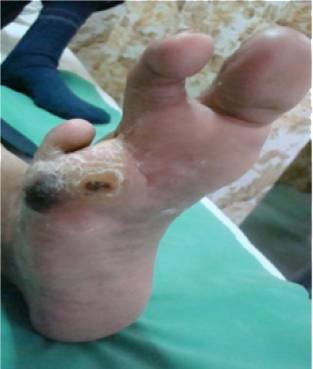
19 patients [90.48%] with osteomyelitis had
underlying ulcers [Figure 1] and these were
type 3 diabetic foot complication whereas 2
patients [9.52%] did not have ulcers but
abscess and they belonged to type 1 diabetic
foot
Figure 1 showing a non healing ulcer with abscess in diabetic foot.
Most common type of diabetic foot osteomyelitis was type 1 osteomyelitis with 12 patients
[57.14%] followed by type 3 osteomyelitis[Table 2] with 5 patients [23.81%].
Table 2 Distribution of Gender according to the Amit Jain’s classification of diabetic foot
Osteomyelitis.
An Analysis of osteomyelitis in Diabetic Foot using Amit jain’s Classification of
Diabetic foot osteomyelitis
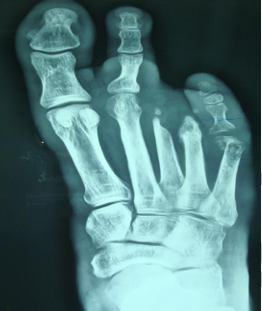
Figure 2 showing the radiograph of patient in figure 1. Note this is type 1-B diabetic foot
osteomyelitis according to Amit Jain’s classification of diabetic foot osteomyelitis affecting the
5th metatarsal.
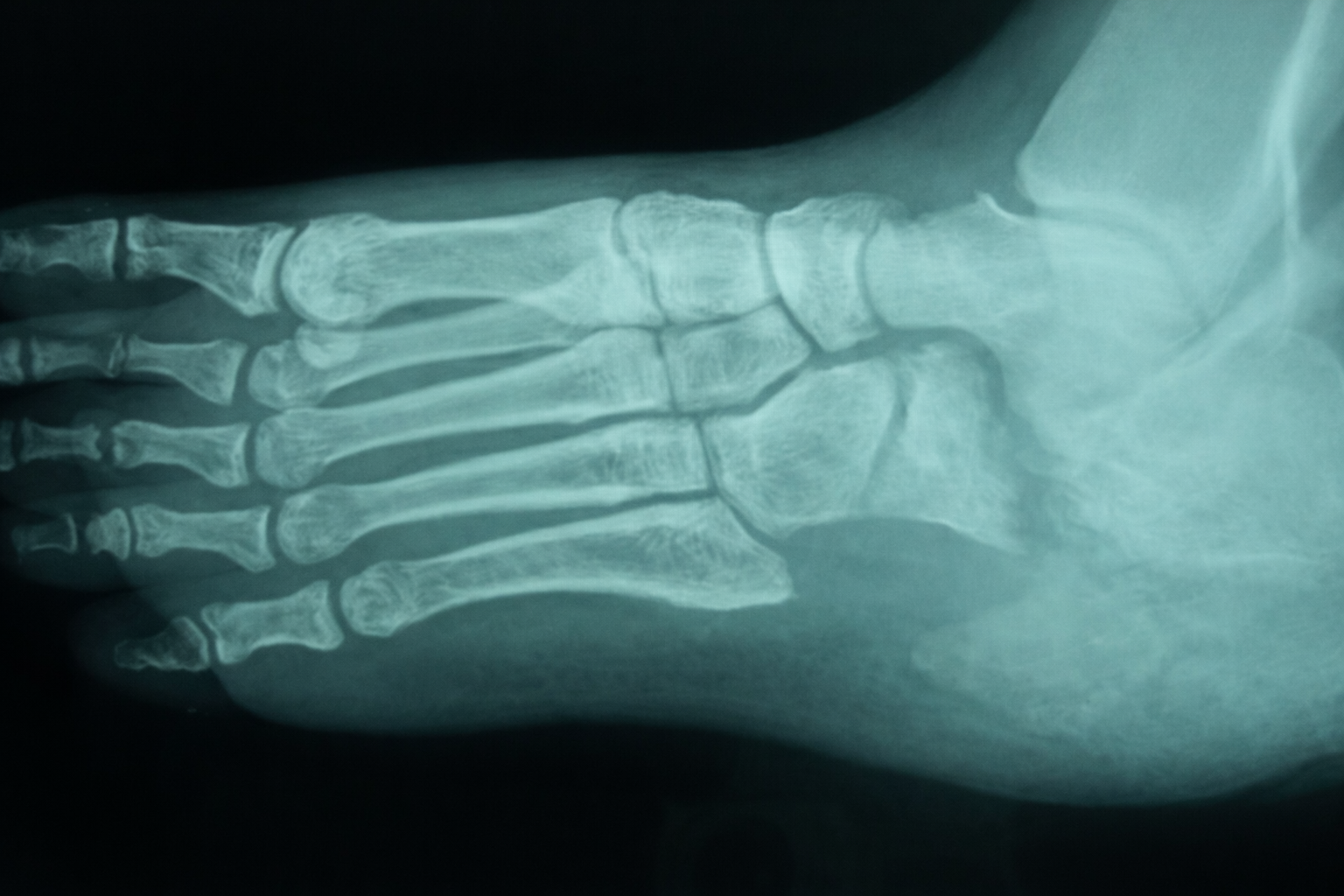
Figure 2showing radiograph of a patient with osteomyelitis of calcaneum. This is type 3-C
diabetic foot osteomyelitis according to Amit Jain’s classification.
2 cases [9.52%] of osteomyelitis had associated charcot foot and they were type 2 osteomyelitis.
There was no mortality in this study and none of the patients had underlying peripheral vascular
disease.
Original article
An Analysis of osteomyelitis in Diabetic Foot using Amit jain’s Classification of
Diabetic foot osteomyelitis
Table 3 showing distribution of cases into different types and subtypes of osteomyelitis
according to Amit Jain’s classification of diabetic foot osteomyelitis.
Around 7 patients [33.33%] with diabetic foot osteomyelitis underwent major amputation [Table
4] with type 3 osteomyelitis being the commonest cause of major amputation.
GENERAL CLASSIFICATION 2 – AMIT JAIN’S OFFLOADING CLASSIFICATION BASED ON AIM OF OFFLOADING
Table 4 showing showing distribution of different surgeries according to Amit Jain’s
classification of diabetic foot osteomyelitis.
DISCUSSION
Diabetic foot osteomyelitis continues to be
one of the most common challenging entities
to diagnose and manage accurately10.
Osteomyelitis and diabetic foot infection are
common entities with serious complications
that can result in lower extremity
amputation11.
Osteomyelitis should always be considered
when the ulcer fails to heal1. Infact,
osteomyelitis in diabetic foot occurs via
contiguous spread from an adjacent infected
wound in 94% of the cases2. In our study, all
cases of osteomyelitis were due to local
pathology, with 90.48% cases having
underlying ulcer. Such cases belong to type
3 diabetic foot complications12.
Various classifications have been suggested
for osteomyelitis in general of which
Waldogel and Cierny- Mader are the two
most commonly employed classification13,
14. Amit Jain’s classification for diabetic
foot osteomyelitis15, 16 is a new classification
specific for diabetic foot osteomyelitis.
Around 90% of diabetic foot ulcers are
known to occur in forefoot, 1.5% in the
midfoot and 4.5% in the calcaneus1. Hence,
forefoot is the most likely involved
anatomical region for osteomyelitis. Around
7-8% of the cases have calcaneal
osteomyelitis17, 18.
In our study, 57.14% had forefoot
osteomyelitis [type 1 diabetic foot
Original article
An Analysis of osteomyelitis in Diabetic Foot using Amit jain’s Classification of
Diabetic foot osteomyelitis
osteomyelitis] and 23.81% had type 3
osteomyelitis which involved calcaneum.
The possible reason for such a high
incidence
of
hindfoot
osteomyelitis
compared to that in the literature is due to
the fact that most physicians avoid treating
calcaneal osteomyelitis and refer to higher
centre or specialist surgeon for further
management as the results with hindfoot
osteomyelitis are not quite favourable.
Diagnosis of osteomyelitis can sometimes
be difficult in diabetic foot, especially in
early cases11, 19, where x rays may not show
any changes. In such cases magnetic
resonance imaging {MRI} or bone
scintigraphy may be required. MRI has been
shown to have the highest sensitivity and
specificity
[>90%]
for
diagnosing
osteomyelitis2. The only problem occurs
when one has to distinguish osteomyelitis
from charcot foot5. In our study, 9.52% of cases had charcot
foot along with osteomyelitis. In one study6,
64.3% of patients with osteomyelitis had
underlying peripheral vascular disease
whereas in our study, none of the patient had
peripheral vascular disease. It is quite
obvious due to the fact that majority of
diabetic foot patients in India suffer from
neuropathy and infection16, 20. Management of diabetic foot osteomyelitis
varies from centre to centre and region to
region5. Some specialist believes in
management
of
osteomyelitis
with
antibiotics alone whereas some believe in
early surgical treatment5. Conservative
surgery1, 6 is defined as procedure in which
no amputation of any part of the foot is
undertaken and includes debridement of non viable/infected tissues and bones. Major
amputation includes below knee and above
knee amputation. In literature, major
amputation from osteomyelitis ranges from
8 – 25%4, 5, 6, 11. In our study, 33.33% had
major amputation whereas only 28.57% had
conservative surgical approach. There was
no mortality in our series.
This study on osteomyelitis using Amit
Jain’s
classification
osteomyelitis provides a better insight on
osteomyelitis
and
for diabetic foot
henceforth
the
classification would help to form a better
communication tool. This new classification
is one of the component of Amit Jain’s
Principle and Practice of diabetic foot
consisting of newer concepts in diabetic foot
like typings, grading and scoring the
diabetic foot complications to improvise and
standardize the practice of diabetic foot
around the world12, 16, 21, 22, 23.
Original article
An Analysis of osteomyelitis in Diabetic Foot using Amit jain’s Classification of
Diabetic foot osteomyelitis
type of osteomyelitis the patient is affected
commonly and also the type of osteomyelitis
responsible for major amputation.
REFERENCES
Crim BE, Wukich DK. Osteomyelitis of the foot and ankle in the diabetic population: Diagnosis and treatment. J Diab Foot Comp. 2009;1(2):26–35.
Nube V, Bolton T, Chua E, Yue D. Osteomyelitis in the diabetic foot: What lies beneath. Primary Intention. 2007;15(2):49–57.
Solagberu BA. A new classification of osteomyelitis for developing countries. East Afr Med J. 2003;80(7):373–378.
Game F. Management of osteomyelitis of foot in diabetes mellitus. Nat Rev Endocrinol. 2010;6:43–47.
Game FL. Osteomyelitis in the diabetic foot: Diagnosis and management. Med Clin North Am. 2013;97:947–956.
Aragon-Sanchez FJ, Cabrera-Galvan JJ, Quintana-Marrero Y, et al. Outcomes of surgical treatment of diabetic foot osteomyelitis: A series of 185 patients with histopathological confirmation of bone involvement. Diabetologia. 2008;51(11):1962–1970.
Shah SF, Hameed S, et al. Evaluation and management of diabetic foot: A multicentric study conducted at Rawalpindi and Islamabad. Ann Pak Inst Med Sci. 2011;7(4):233–237.
Muqim RU, Griffin S, Ahmed M. Evaluation and management of diabetic foot according to Wagner’s classification: A study of 100 cases. J Ayub Med Coll Abbottabad. 2003;15(3):39–42.
Solanki K, Parmar H, Gohil V, Shah S. The surgical management of diabetic foot. NJIRM. 2010;1(4):1–3.
Hoffman WB, Khan KH, Kosinski M. Current concepts in treating diabetic foot osteomyelitis. Podiatry Today. 2009;22(10):1–7.
Widatalla AH, Mahadi SEI, Shawar MA, et al. Diabetic foot infections with osteomyelitis: Efficacy of combined surgical and medical treatment. Diabetic Foot & Ankle. 2012;3:1–6.
Jain AKC. A new classification of diabetic foot complications: A simple and effective teaching tool. J Diab Foot Comp. 2012;4(1):1–5.
Carek PJ, Dickerson LM, Sack JL. Diagnosis and management of osteomyelitis. Am Fam Physician. 2001;63(12):2413–2421.
Mader JT, Shirtliff M, Calhoun JH. Staging and staging application in osteomyelitis. Clin Infect Dis. 1997;25:1303–1309.
Jain AKC. A new classification of diabetic foot osteomyelitis. OA Case Reports. 2013;2(3):121.
Kalaivani V, Vijayakumar HM. Diabetic foot in India: Reviewing the epidemiology and Amit Jain’s classifications. Sch Acad J Biosci. 2013;1(6):305–308.
Wang EHM, Simpson S, Bennett GC. Osteomyelitis of the calcaneum. J Bone Joint Surg. 1992;74-B:906–909.
Bhattacharyya A, Das R. Gaenslen’s split heel approach for treatment of chronic osteomyelitis of the calcaneus: A series of three cases. FAOJ. 2010;3(11):3.
Lipsky BA. Osteomyelitis of the foot in diabetic patients. Clin Infect Dis. 1997;25:1318–1326.
Jain AKC, Viswanath S. Distribution and analysis of diabetic foot. OA Case Reports. 2013;2(12):117.
Jain AKC. The new scoring system for predicting the risk of major amputations in patients with diabetic foot complications. Med-Science. 2014;3(1):1068–1078.
Jain AKC. A new classification (grading system) of debridement in diabetic lower limb: An improvisation and standardization in practice of diabetic limb salvage around the world. Med-Science. 2014;3(1):991–1001.
Jain AKC. A new staging system for cellulitis in diabetic lower limbs: Improvising diabetic foot practice around the world. J Diab Foot Comp. 2014;6(2):48–53.
AUTHORS’ CONTRIBUTIONS
Dr Amit Kumar- Data collection, Conceptualization, design and preparation of manuscript. Dr
Viswanath – critical revision and data collection.